This one catches people completely off guard.
You are not dealing with a new product, a procedure gone wrong, or a sun exposure mistake. Your routine has not changed. Nothing external has changed. But your skin has. Pigmentation is appearing in places it was not before, or existing patches are shifting in ways you cannot explain. And the cause might not be in your skincare at all. It might be in your thyroid.
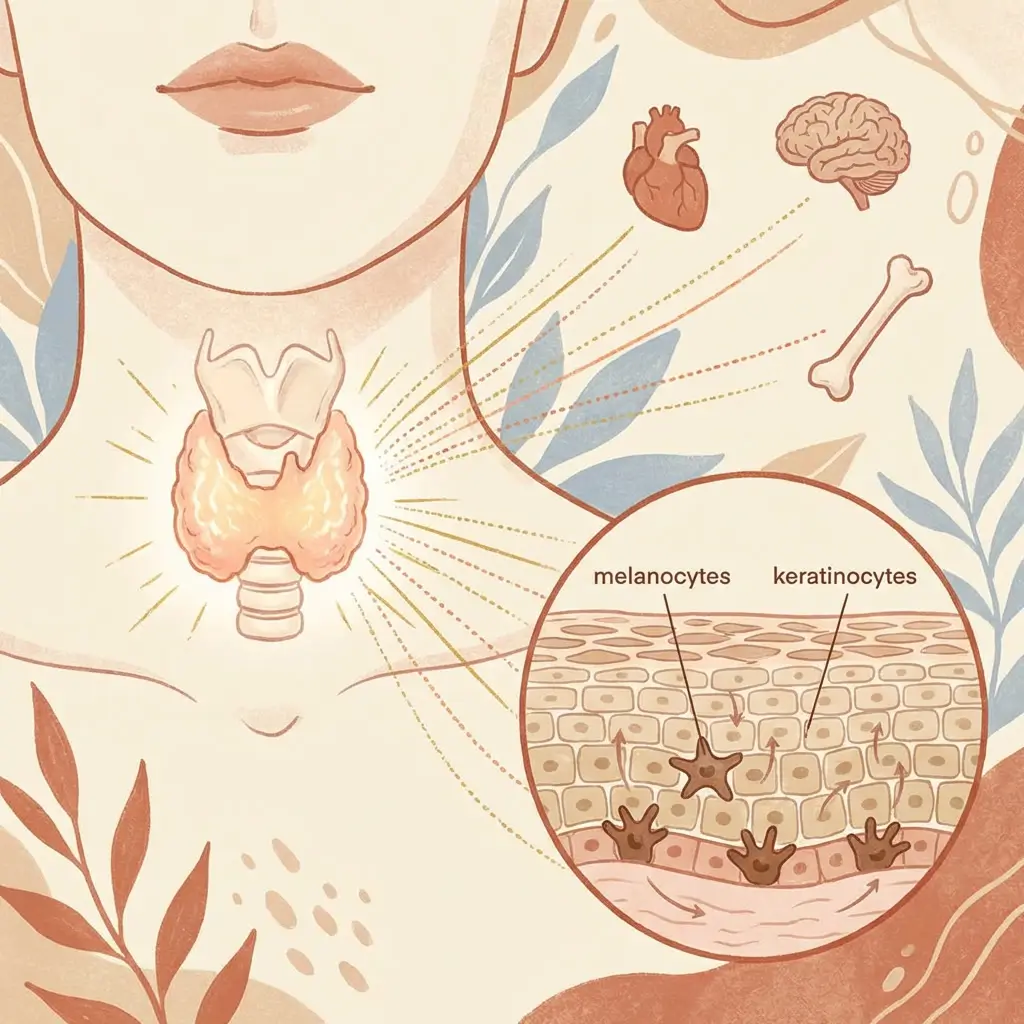
Your thyroid is a small gland at the base of your neck, and it controls the metabolic speed of virtually every cell in your body. That includes your melanocytes and the keratinocytes that carry pigment to the surface. When thyroid function shifts, your skin's entire operating tempo changes with it, and pigmentation is one of the most visible places that shows up.
The basics of how your thyroid talks to your skin
Your thyroid produces hormones (primarily T3 and T4) that regulate how fast cells work, divide, and turn over. When thyroid levels are normal, everything hums along at the right pace. Skin cells are produced, migrate to the surface, carry their pigment load, and shed on a predictable cycle. Melanocytes produce pigment at a steady, regulated rate.
When thyroid function is too low (hypothyroidism) or too high (hyperthyroidism), that tempo changes. And the downstream effects on pigmentation are different depending on which direction the imbalance goes.
This is not a dramatic, overnight shift like pregnancy hormones flooding your system. Thyroid changes tend to be gradual, which is why the skin changes they produce often go unrecognised for months. The pigmentation creeps in slowly enough that you adjust to it, and by the time you notice, the connection to something systemic is not obvious. This gradual, hard-to-pin-down quality is one of the reasons thyroid-driven pigmentation often falls into the category of stubborn hyperpigmentation that resists topical treatment.
How hypothyroidism affects pigmentation
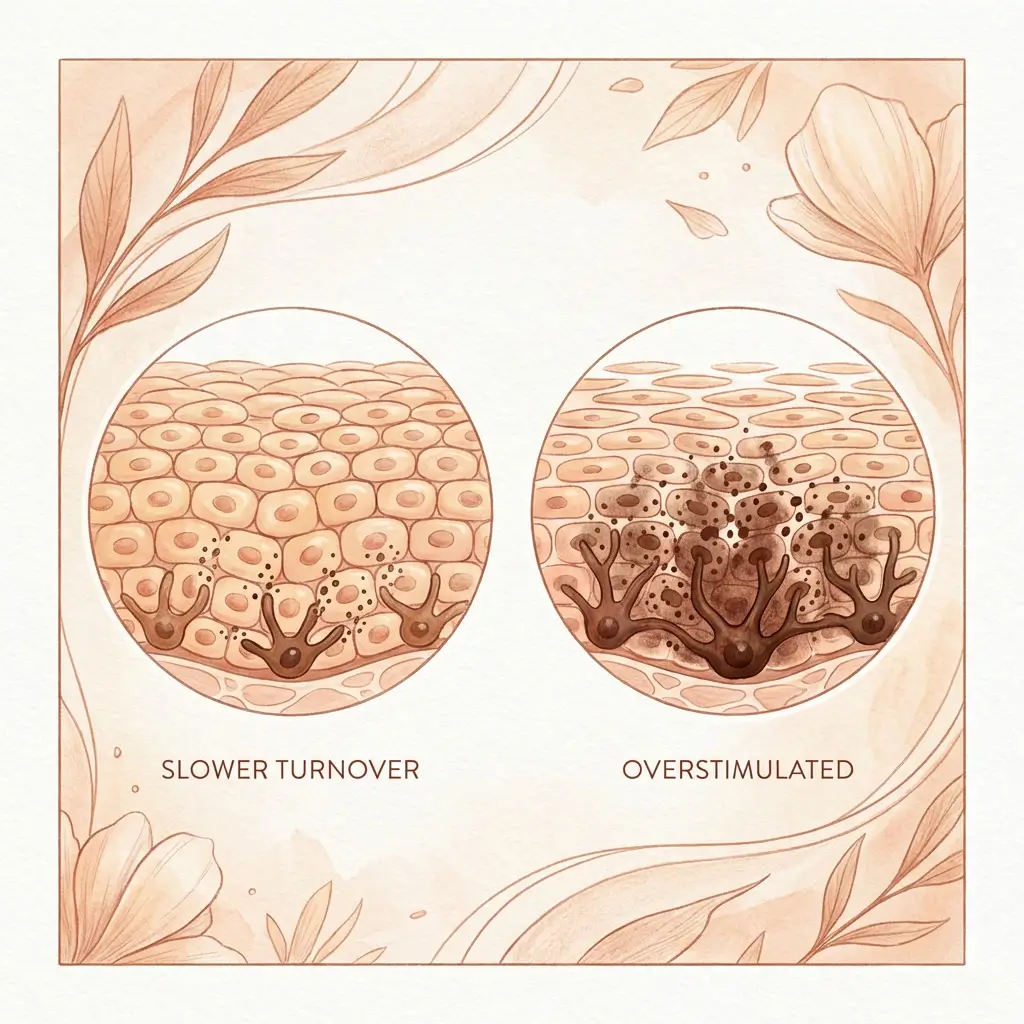
When the thyroid is underactive, everything slows down. Cell division slows. Skin turnover slows. And the consequences for pigmentation play out in a few specific ways.
Pigmented cells stay longer
In healthy skin, keratinocytes that have received melanin from melanocytes migrate to the surface and eventually shed. That turnover is what keeps pigmentation from accumulating. When thyroid function drops, that turnover rate decreases. Pigmented cells sit in the skin for longer before being replaced. Marks that would normally fade over weeks linger for months. Areas that were lightly pigmented become more visibly so, simply because the pigment is not being cleared at the usual rate.
This can look like your skin is producing more pigment when in reality it is just holding on to what it already has.
Increased melanocyte sensitivity
Hypothyroidism alters the hormonal environment in ways that go beyond thyroid hormones alone. TSH (thyroid-stimulating hormone) rises when the thyroid is underactive, and TSH shares structural similarities with melanocyte-stimulating hormone (MSH). At elevated levels, TSH can cross-react with melanocyte receptors and directly stimulate pigment production.
There is also an indirect pathway. Hypothyroidism tends to increase systemic inflammation and oxidative stress, both of which create the internal conditions that make melanocytes more reactive to other triggers. UV exposure, friction, and hormonal fluctuations that your skin might have handled without visible pigment changes can start producing a response, because the melanocytes are now operating in a more inflammatory, less regulated internal environment.
This overlap is important. Thyroid dysfunction rarely operates in isolation. It frequently co-occurs with stress-driven hormonal imbalance, blood sugar dysregulation, and gut dysfunction, all of which independently affect melanocyte behaviour. When several of these are present at once, the pigmentation becomes harder to trace to a single cause, because the triggers are reinforcing each other.
Diffuse darkening
One of the characteristic pigment presentations in hypothyroidism is a generalised, diffuse darkening rather than the defined patches you see with melasma or PIH. The skin can take on a slightly yellowish or brownish tone, particularly on the face. Understanding whether you are looking at diffuse pigmentation versus a patch-based pattern matters, because it changes the likely cause and the appropriate response.
This presentation can also overlap visually with skin redness and inflammation masquerading as pigmentation, particularly in the early stages.
How hyperthyroidism affects pigmentation
An overactive thyroid pushes everything faster. Cell turnover accelerates. Metabolic rate increases. And while you might expect faster turnover to clear pigment more efficiently, the reality is more complicated.
Melanocyte overstimulation
Hyperthyroidism increases the levels of thyroid hormones circulating in your body, and thyroid hormones directly influence melanocyte activity. Excess T3 and T4 can stimulate melanocytes to produce more pigment, particularly in areas that are already prone to pigmentation: the face, neck, skin folds, and areas of friction.
The stimulation pattern is different from hypothyroidism. Where an underactive thyroid produces a slow, diffuse change, an overactive thyroid can produce more noticeable, faster-onset darkening, particularly in specific areas.
Localised hyperpigmentation patterns
Hyperthyroidism is associated with darkening of the skin in characteristic locations: around the eyes (periorbital hyperpigmentation), on the shins (sometimes associated with thyroid dermopathy), and in skin folds and friction areas. These patterns are well documented clinically but not always connected to thyroid function by the person experiencing them, especially when they appear before other thyroid symptoms become obvious.
Heat and sweating compound the effect
Hyperthyroidism increases body temperature and sweating. Both of these independently affect melanocyte behaviour. Heat is a direct melanocyte stimulator through a pathway that operates separately from UV. Excessive sweating can irritate the skin, particularly in folds and friction areas, creating an additional inflammatory signal on top of the hormonal one. When you layer hormonal overstimulation, heat activation, and friction-driven inflammation, you get a compound trigger that is stronger than any of those inputs alone.
Why pigment changes can be an early signal
This is the part worth paying real attention to.
Thyroid dysfunction often develops gradually. The classic symptoms (fatigue, weight changes, hair thinning, temperature sensitivity) can take months to become noticeable or can be attributed to stress, aging, or lifestyle. In the early stages, blood work may even come back in the "normal" range while the thyroid is already shifting.
Skin changes, including pigmentation shifts, can be among the first visible signs. The skin responds to hormonal changes with surprising sensitivity, and because you look at your face every day, you may notice a pigmentary shift before you notice the fatigue or the weight change.
This does not mean that every unexplained pigment change points to your thyroid. But if you are experiencing pigmentation changes that do not have an obvious external trigger, especially in combination with any of the following, thyroid function is worth investigating:
- Fatigue that does not improve with rest
- Unexplained weight gain or loss
- Hair thinning, particularly at the outer edges of the eyebrows
- Dry skin or skin texture changes beyond the pigmentation
- Feeling consistently too cold or too hot
- Changes in your menstrual cycle
- Increased stress sensitivity or mood changes
A simple blood test (TSH, free T3, free T4) can identify or rule out thyroid dysfunction. If your pigmentation turns out to be thyroid-related, addressing the thyroid imbalance is the single most important step, because the pigment changes are downstream of the hormonal problem, and treating them topically without correcting the source will not produce lasting results.
Why melanin-rich skin shows it more
The same principle applies here as with every other hormonal and inflammatory trigger: melanocytes in melanin-rich skin are more responsive to stimulation and produce a more visible output from the same input.
Thyroid-related pigmentation changes that might be undetectable in lighter skin can produce clearly visible darkening in deeper skin tones. The diffuse pigmentary shift of hypothyroidism is more noticeable. The localised darkening patterns of hyperthyroidism are more pronounced. And because thyroid conditions are often underdiagnosed in women of colour (symptoms are attributed to other causes, and some clinical signs like skin pallor are harder to assess in darker skin), the pigmentation changes may go unexplained for longer.
If you have melanin-rich skin and are experiencing pigmentation that does not fit the usual patterns (not clearly PIH, not clearly melasma, not tied to a product or procedure), a thyroid check is a reasonable and underutilised step.

What to take from this
Thyroid dysfunction is not the most common cause of hyperpigmentation, but it is one of the most overlooked. It produces pigment changes that are gradual, diffuse, and easy to misattribute to aging, sun damage, or products. And because it is systemic, no amount of topical treatment will fully resolve pigmentation that is being driven by an underlying thyroid imbalance.
It also rarely acts alone. Thyroid dysfunction creates downstream effects on inflammation, stress hormones, blood sugar regulation, and gut health, all of which feed into melanocyte behaviour through their own pathways. That interconnection is what makes thyroid-related pigmentation feel so stubborn and confusing. It is not one trigger. It is one trigger that destabilises several others.
The value of knowing about this connection is not that you should assume your pigmentation is thyroid-related. It is that you should not rule it out, particularly if the pattern does not match the usual types. Unexplained pigmentation changes, especially in combination with other subtle symptoms, are worth investigating from the inside, not just treating from the outside.
Sometimes the answer is not on your bathroom shelf. It is in your bloodwork.






