Your dark spots are not random. Every single one of them started the same way: a stress signal reached your skin, and the cells responsible for pigment responded. Sometimes that signal came from the outside (sun, heat, friction). Sometimes it came from the inside (hormones, inflammation, a nutrient gap you did not know you had). Either way, your melanocytes got the message and started producing.
That is the part nobody explains properly. So here it is, all of it, in one place.
How pigment is actually made
Your skin contains specialised cells called melanocytes sitting at the base of the epidermis. Their job is to make melanin, the pigment that gives your skin its colour and protects your DNA from damage.
Under normal conditions, they produce at a steady rate. Your baseline skin tone is the result.
When a stress signal hits, the process ramps up:
- A trigger arrives (UV, heat, inflammation, hormones, anything your body reads as a threat)
- An enzyme called tyrosinase activates (this is the rate-limiting step, the bottleneck that controls how much melanin gets made)
- Melanin is produced and packaged into structures called melanosomes
- Melanosomes transfer upward into surrounding skin cells, where they sit as visible pigment
When you treat only the surface, pigment reappears because the trigger underneath is still sending signals.
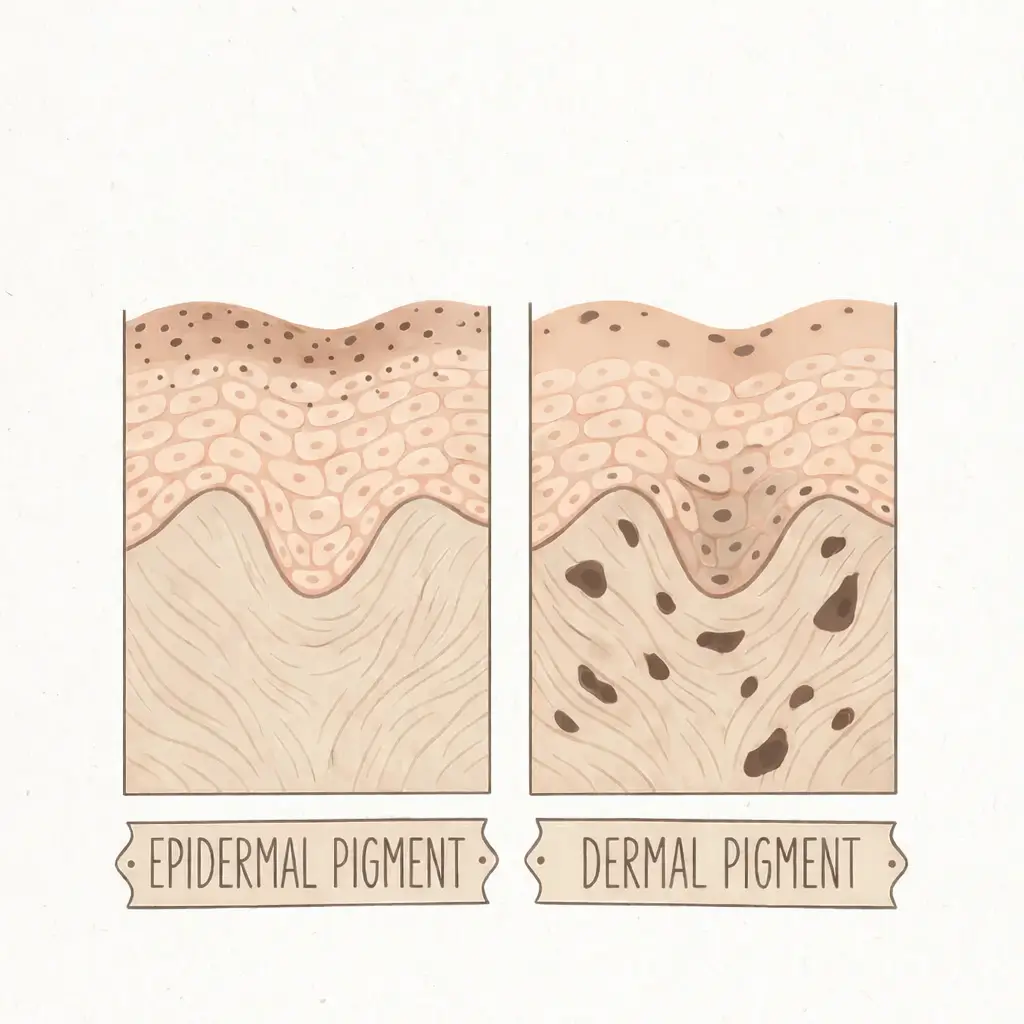
Where that melanin ends up also changes everything about how long it sticks around:
| Epidermal pigment | Dermal pigment | |
|---|---|---|
| Colour | Brown, tan, dark brown | Blue-grey, ashy, muted |
| Depth | Upper skin layers | Deeper dermis |
| Edges | More defined | More diffuse |
| Response to topicals | Faster, more visible | Slow or minimal |
| Cleared by | Normal skin turnover | Macrophage removal |
| Typical timeline | Weeks to months | Months to years |
This is why two people with similar-looking marks can have completely different fading timelines. It is not about effort or product quality. It is about where the pigment ended up.
The one thing nearly every trigger has in common
Before we get into the individual triggers, this is worth knowing first.
Nearly every cause covered here, whether it is UV, heat, acne, friction, hormones, or stress, activates pigment through the same biological mechanism: inflammation.
Stressed, damaged, or irritated skin sends out inflammatory signals. Melanocytes read those signals as a call to produce. That is the shared pathway underneath almost all hyperpigmentation.
Why does this matter? Because it changes the logic of treatment entirely. If inflammation is the common thread, then calming inflammation is not one step in a plan. It is the foundation. Before the serum. Before the procedure. Before the retinoid.
If you have melanin-rich skin, this is especially relevant. Your melanocytes respond faster, produce more melanin, and react to a wider range of triggers. That is not a flaw. It is your skin doing what it evolved to do, at a higher volume. But it means anything creating inflammation in or around your skin carries a higher pigment risk, and treatment approaches that create their own inflammation (aggressive peels, high-strength acids, certain lasers) can backfire.
Identify your primary trigger
Most people have more than one trigger contributing. But one usually dominates. Start there.
If your pigment worsens after time outdoors, near heat, or in bright indoor light... You are likely dealing with energy and environmental triggers. This is the most universal category. UV, visible light, and heat all activate melanocytes through different pathways, and they stack. Even without a visible sunburn.
If your marks are the shadows left after acne, a rash, or a procedure... This is post-inflammatory hyperpigmentation (PIH), one of the most common forms. The pigment is not from the breakout itself. It is from the inflammatory response it triggered. The worse the inflammation, the darker and longer-lasting the mark.
If pigment appears where you shave, wax, or experience friction... Mechanical stress is your trigger. Bra straps, waistbands, repeated rubbing. The darkening is not from the contact. It is from the chronic low-level inflammatory response the contact generates.
If your pigment flares with your cycle, during pregnancy, or when stress and sleep are off... Internal signals are likely contributing. Hormonal shifts, cortisol, blood sugar dysregulation, and sleep disruption all generate systemic inflammation that reaches your melanocytes through the bloodstream. Nothing touched your skin. But something shifted inside.
If your pigment appeared or worsened after starting a new product... Your skincare routine might be the trigger. Over-exfoliation, aggressive actives, and barrier damage create the exact same inflammatory signalling as every other trigger listed above. The irony of skincare causing the problem it is trying to solve is more common than most people realise.

Deep-dive guides by trigger
Each category below gets a brief explanation of the biology, followed by the detailed articles that go deeper.
Energy and environmental exposure
UV is the most universal trigger, but it is not the only one. UVA penetrates into the dermis and activates melanocytes through oxidative stress. UVB causes more acute surface damage. Visible light (especially blue/HEV light) activates melanocytes through a completely separate opsin receptor pathway, and this effect is significantly stronger in melanin-rich skin. Heat activates pigment independently of light entirely, through vascular and inflammatory signalling.
Four separate mechanisms. All additive. All often happening at the same time.
- How UV Exposure Activates Hyperpigmentation
- How Visible Light (HEV) Activates Hyperpigmentation
- How Heat Exposure Activates Hyperpigmentation
- How Sunburn Triggers Hyperpigmentation (and Why It Often Lingers)
Inflammation and injury
Any inflammatory event in the skin can activate melanocytes at the site. Acne, eczema flares, allergic reactions, cosmetic procedures. The deeper or more sustained the inflammation, the darker and more persistent the mark. In melanin-rich skin, even mild inflammation can produce visible pigment changes. This is the mechanism behind PIH, and it is also why procedures designed to improve pigmentation sometimes make it worse.
- How Acne-Related Inflammation Triggers Hyperpigmentation
- How Eczema and Skin Flares Trigger Hyperpigmentation
- How Post-Procedure Inflammation Triggers Hyperpigmentation
Mechanical stress
Friction, pressure, and repetitive contact create micro-inflammation that trips the same pigment pathway. The darkening under bra straps is not from the fabric. It is from what the fabric is doing to your skin's inflammatory signalling, day after day.
Skincare and routine-induced irritation
The trigger nobody wants to hear about. Over-exfoliation, acids at too-high concentrations, retinoids introduced too fast, damaged barrier function. Your skin can look like it is responding to treatment while actually being pushed into producing more pigment. If your routine stings every time you apply it, that is not "working." That is a new trigger.
Hormonal and metabolic signals
Estrogen and progesterone directly increase melanocyte sensitivity. This is why pigmentation commonly appears during pregnancy, with hormonal contraceptives, and around perimenopause. It is the primary mechanism behind melasma, which behaves very differently from PIH and usually needs a different approach. Thyroid dysfunction and insulin resistance also influence pigment through their effects on inflammation, turnover, and cellular metabolism.
- How Pregnancy-Related Hormonal Shifts Trigger Hyperpigmentation
- How Birth Control Changes Trigger Hyperpigmentation
- How Thyroid-Related Signals Trigger Hyperpigmentation
- How Blood Sugar Regulation Affects Hyperpigmentation
Stress, sleep, and internal load
Chronic stress keeps cortisol elevated. Elevated cortisol keeps inflammatory signalling active. Active inflammatory signalling keeps melanocytes reactive. Poor sleep makes all of it worse by disrupting the repair cycles your skin depends on to resolve pigment. These are not fringe factors. They explain why dark marks can worsen during a rough month even when the skincare routine has not changed.
Gut function and nutrient availability
Gut dysfunction (poor absorption, permeability, dysbiosis) and nutrient gaps (iron, B vitamins, zinc, vitamin D) reduce your skin's capacity to regulate pigment and repair effectively. For most people, these are contributing factors rather than primary triggers. But if you have addressed the obvious causes and your pigment is still not budging, internal nutritional status is worth investigating.

When pigment will not budge
If your pigment feels stuck despite consistent effort, the issue is usually not the products. It is one of these:
- The original trigger is still active (and you may not realise it)
- The pigment has dropped into the dermis, where topicals cannot reach it
- Multiple triggers are layered, and you are only addressing one
- The timeline expectation does not match the biology (dermal pigment can take 6 to 24 months)
- Something internal is contributing alongside the external triggers
These articles unpack each of those patterns:
- Why Hyperpigmentation Often Looks Darker Before It Fades
- What Makes Hyperpigmentation Stubborn (Even With Consistent Skincare)
- The Role of Inflammation in Hyperpigmentation
Common mistakes
Confusing irritation with progress. If your skin stings, reddens, or peels every time you use an active, that is not "purging" or "adjusting." Irritation is inflammation. Inflammation activates melanocytes. You are creating a new trigger while trying to treat the old one.
Treating one trigger while ignoring the others. Sun exposure layered on top of hormonal sensitivity is extremely common. Addressing only the UV while the hormonal signal runs in the background means the pigment keeps returning. Most persistent hyperpigmentation involves at least two categories.
Overlooking invisible exposure. Visible light and heat do not always feel intense, but they still activate pigment signalling, especially in melanin-rich skin. Indoor light through windows, laptop heat on your legs, warm environments you sit in daily. These are frequently the triggers nobody considers.
FAQ
What causes hyperpigmentation on the face?
UV exposure, hormonal signalling, and post-inflammatory pigment from acne or irritation are the three most common drivers. Most women dealing with persistent facial pigmentation have at least two contributing at the same time.
Can stress cause hyperpigmentation?
Yes. Chronic stress keeps cortisol elevated, which maintains the inflammatory signalling that keeps melanocytes reactive. Pigment can worsen during stressful periods even when nothing has changed about sun exposure or skincare.
Why did my dark spots suddenly get worse?
Usually one of four things: increased UV or heat exposure (including seasonal changes), a hormonal shift, a new skincare product irritating the skin, or a spike in stress and sleep disruption.
Does heat cause hyperpigmentation?
Yes. Heat activates melanocyte signalling through inflammatory and vascular pathways that have nothing to do with UV. Cooking over a stove, laptops on the legs, saunas, hot climates. One of the most under recognised triggers, especially for melasma.
Is hyperpigmentation genetic?
Genetics determines how responsive your melanocytes are, not whether you get hyperpigmentation. People with melanin-rich skin have melanocytes that react faster and more intensely. That is a genetic trait, not a disorder. The triggers themselves are environmental, hormonal, and behavioural.
What is the difference between PIH and melasma?
PIH is pigment left after a specific inflammatory event like a breakout or irritation. Melasma is a hormonal pattern worsened by UV, visible light, and heat. PIH is tied to a clear trigger and location. Melasma tends to appear symmetrically on the cheeks, forehead, upper lip, and jawline. They respond to different treatment approaches and have different recurrence patterns.
Where to go next
Figure out your pigment type. PIH, melasma, sun spots, and post-procedure pigmentation all respond differently. Hyperpigmentation types helps you confirm what you are actually dealing with.
Look at treatment options. Once you know your trigger and your type, hyperpigmentation treatments covers topical approaches, professional procedures, and the internal strategies that address what topicals cannot reach.
The mark on your skin is the end of a chain reaction, not the beginning. Trace it back to the signal, and you stop repeating the cycle.


