You already know stress is bad for your skin. That is not new information. What most people do not realise is how it is bad for it, specifically when it comes to pigmentation, and why poor sleep makes the same problem worse through a connected but distinct mechanism.
Stress and sleep disruption are not background noise. They are active triggers. They maintain the inflammatory conditions that keep melanocytes reactive, slow down the repair processes that clear pigment, and lower the threshold at which everything else (UV, friction, hormones, products) produces a visible mark.
If your pigmentation seems to flare during difficult periods and improve when life calms down, that is not coincidence. It is physiology.
What chronic stress does to your skin's pigment system
Acute stress is brief. Your body activates, cortisol rises, the threat passes, cortisol falls, everything resets. Your skin barely notices.
Chronic stress is different. The threat does not pass. Cortisol stays elevated. And when cortisol stays elevated, it stops being a useful short-term response and starts reshaping the environment your body operates in.
For pigmentation, there are two things that matter.
It raises your inflammatory baseline
Cortisol is supposed to be anti-inflammatory in the short term. That is one of its functions during acute stress. But when it is elevated chronically, the relationship inverts. Tissues become less responsive to cortisol's anti-inflammatory effects (a kind of cortisol resistance), and the net result is a sustained increase in systemic inflammatory signalling.
This is the same inflammatory environment that drives pigmentation after a breakout, a procedure, or a product reaction. The difference is that with stress, the inflammation is not coming from a specific injury to a specific area. It is ambient. It is everywhere. And it does not resolve on its own, because the source is still active.
Your melanocytes sit in that environment constantly. They are not being hit with a loud, specific signal. They are receiving a low, steady hum of inflammatory mediators that keeps them primed. The result is not dramatic, sudden pigmentation. It is a gradual lowering of the threshold. Triggers that your skin used to handle without marking start leaving marks. Pigment that should be fading holds on longer. New patches appear in places that do not seem connected to anything you are doing on the surface.
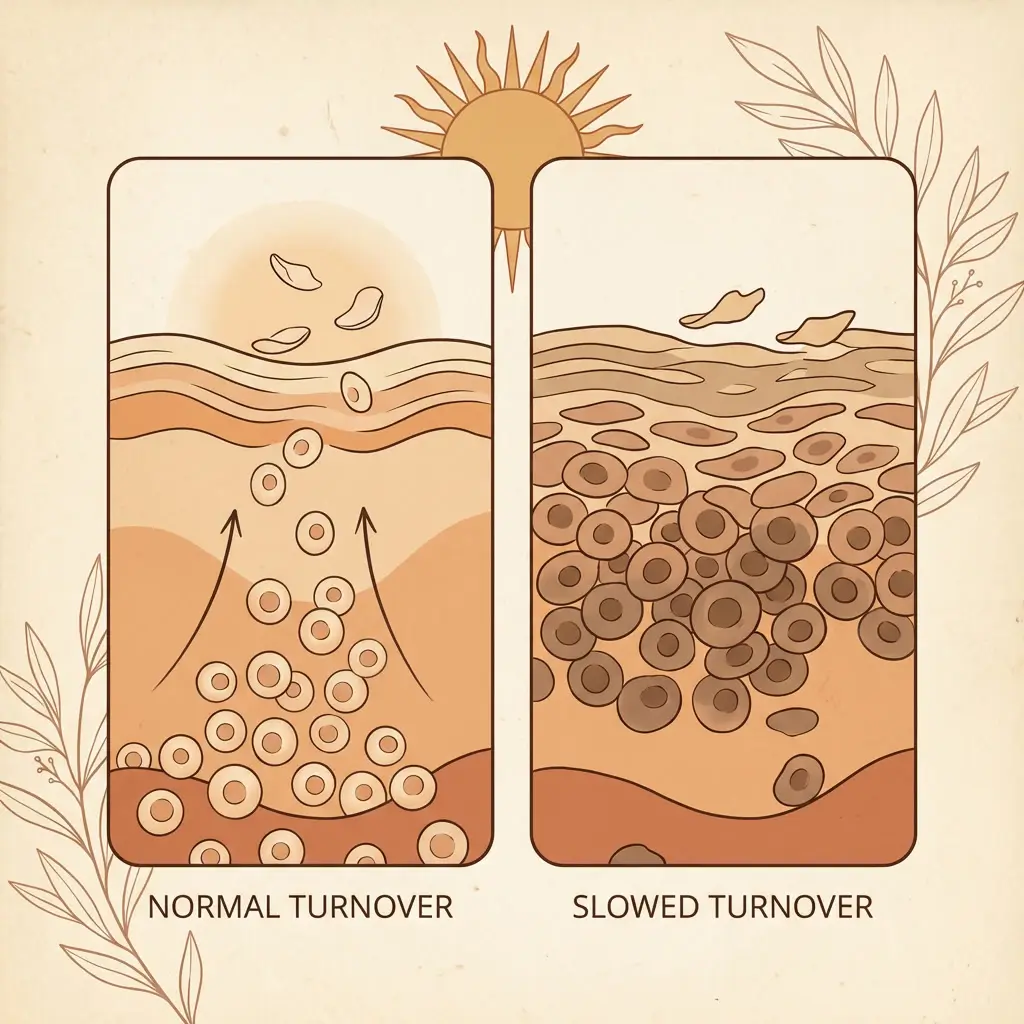
It slows everything down
Cortisol suppresses the processes your skin needs to repair and renew itself. Cell turnover slows. Collagen production drops. Barrier function weakens. Wound healing takes longer.
For pigmentation specifically, slower turnover means pigmented keratinocytes (the cells that carry melanin to the surface) sit in the skin longer before being shed. Marks that would normally fade over weeks linger for months. The pigment is not being produced faster necessarily. It is just not being cleared at the rate it should be.
This is why pigmentation seems to stall under chronic stress. You can be doing everything right in your routine and still feel like nothing is moving. The treatments are working. The skin just cannot process the results at normal speed.
How chronic stress keeps hyperpigmentation active covers the full cortisol and HPA axis mechanism.
What poor sleep adds to the picture
Sleep disruption is not just a symptom of stress. It is its own trigger, with its own pathway into melanocyte behaviour. The two overlap, but they are not the same thing, and poor sleep can drive pigmentation even when stress levels feel manageable.
Your skin repairs itself during sleep
Skin cell turnover, DNA repair, collagen synthesis, and barrier restoration all peak during sleep, specifically during deep sleep stages. This is not metaphor. It is measurable. Growth hormone release, which drives much of this repair, is concentrated in the first half of the night during slow-wave sleep.
When sleep is shortened, fragmented, or consistently poor quality, these repair windows shrink. The skin gets less time to do the work it needs to do. Pigmented cells are shed more slowly. Barrier damage from the day is not fully repaired by morning. Inflammation from whatever happened during the day carries over into the next day instead of being resolved overnight.
Over time, this creates a deficit. The skin falls behind on maintenance. Pigmentation that should be gradually clearing is not being cleared efficiently because the overnight repair cycle that drives clearance is compromised.
Circadian disruption affects melanocytes directly
Your skin operates on a circadian rhythm. Melanocyte activity, inflammatory signalling, cell division, and barrier permeability all fluctuate on a 24-hour cycle. This rhythm is not just driven by light and dark. It is encoded in the cells themselves.
When your circadian rhythm is disrupted (irregular sleep schedules, shift work, screen exposure late at night, consistently insufficient sleep), the timing of these processes shifts. Inflammatory pathways that should be winding down at night stay active. Repair processes that should be ramping up are delayed or truncated.
Research on circadian disruption in skin is still developing, but the pattern is consistent: disrupted circadian signalling is associated with increased inflammation, impaired barrier function, and altered melanocyte activity. The skin does not just need sleep. It needs sleep at predictable times.
How poor sleep and circadian disruption affect hyperpigmentation covers the full repair cycle and what disrupts it.

How stress and sleep compound each other
These are not independent problems. They form a loop.
Chronic stress disrupts sleep. Elevated cortisol at night suppresses melatonin production and makes it harder to fall asleep, stay asleep, and reach the deep sleep stages where repair happens. Poor sleep raises cortisol the next day. Higher daytime cortisol increases stress reactivity, making you more sensitive to stressors that would normally be manageable. That increased stress disrupts the following night's sleep.
For your skin, this loop means the inflammatory load keeps building without adequate repair time to offset it. Each day starts with a slightly higher baseline than the last. Melanocytes stay primed. Pigment clearance stays slow. And the gap between what your treatment routine can achieve and what your skin is actually doing widens.
This is one of the reasons pigmentation can seem to spiral during prolonged stressful periods. It is not one bad night or one stressful week. It is the cumulative effect of the stress-sleep loop running without interruption, gradually shifting the internal conditions further away from what your skin needs to regulate pigment normally.
Why this makes treatment less effective
If you have noticed that your pigmentation responds better to treatment during calm, well-rested periods and seems to stall or worsen during stressful ones, there is a direct biological explanation.
Topical treatments work by influencing processes at the skin surface: inhibiting tyrosinase, accelerating turnover, reducing melanin transfer. They are designed to work within a functioning system. When that system is compromised by chronic stress and poor sleep, the treatments are not failing. The system they depend on is running at reduced capacity.
Tyrosinase inhibitors slow pigment production, but if inflammatory signalling is constantly stimulating melanocytes to produce more, the inhibitor is fighting an upstream current. Retinoids accelerate turnover, but if cortisol is suppressing the same turnover, the retinoid is pushing against a brake. Antioxidants neutralise free radicals, but if oxidative stress from sleep deprivation is generating them faster than the antioxidant can clear them, it is a losing equation.
None of this means your routine is wrong. It means the internal conditions are limiting what the routine can achieve. Addressing stress and sleep does not replace topical treatment. It removes the bottleneck that prevents topical treatment from working at full capacity.
Why melanin-rich skin feels this more
The pattern holds. Melanocytes in melanin-rich skin are more responsive to the ambient inflammatory signals that chronic stress and sleep disruption produce. The same elevation in systemic inflammation that might cause no visible pigment changes in lighter skin can produce noticeable darkening or treatment resistance in deeper skin tones.
This also means the stress-sleep loop has a lower threshold for visible impact. Moderate, sustained stress combined with consistently poor sleep, something millions of women live with as a baseline, can be enough to keep melanocytes in a reactive state in melanin-rich skin even when everything else (routine, sun protection, diet) is well managed.

Recognising the pattern
Stress and sleep disruption are easy to normalise. Most women who are dealing with them do not think of them as "triggers" for anything. They are just how life is.
But there are patterns worth noticing:
- Pigmentation that worsens during high-stress periods and improves during holidays or calmer stretches
- Dark marks that seem to stall mid-fade and stop responding to a routine that was previously working
- New pigmentation appearing without any obvious external trigger (no new products, no sun exposure, no procedures)
- Visible darkening in areas that are also subject to friction or hormonal sensitivity, as if those triggers have been amplified
- Skin that feels more reactive overall, stinging or flushing in response to products it previously tolerated
If several of these are present and you can connect them to a period of sustained stress or disrupted sleep, the internal environment is likely a factor.
The difficulty is that nobody can simply stop being stressed or start sleeping perfectly. These are not switches you flip. But recognising that they are active physiological triggers, not just background lifestyle factors, changes how you evaluate what is happening with your skin. It shifts the question from "why is my routine not working" to "what is my skin working against."
What to take from this
Stress and sleep disruption are not the dramatic, visible triggers that procedures or product reactions are. They are quiet. They work systemically. And because they affect everything gradually rather than causing a single obvious event, they are easy to overlook when you are trying to understand why your pigmentation is not improving.
But the mechanism is real. Chronic cortisol elevation raises inflammatory baseline, suppresses repair, and slows pigment clearance. Sleep disruption compounds it by cutting the repair time your skin depends on and destabilising the circadian rhythms that regulate melanocyte activity. Together, they create an internal environment where pigmentation is easier to trigger and harder to shift.
This does not mean you need to fix your stress and sleep before you can treat your skin. It means that if those factors are present and unaddressed, they are actively limiting what your treatment can achieve. The ceiling on your results is not set by your products. It is set by the conditions your skin is operating in.
Your skin does not exist in a vacuum. It exists in your life. And your life is part of the treatment plan, whether you account for it or not.






